In a previous post I discussed the two simple rules that I ask colleagues to use to test interventions around the management of infections:
- First do no harm
- Second, find and take the positive action
All well and good offering this advice to others, but the challenge was also to me as a clinical microbiologist. In discussions with my colleagues, we agreed that a large number of our E coli bacteramias were probably as a result of urinary associated infection and if we were to make a difference, we needed to take a closer interest in how we managed the output from our three urine laboratories. Every laboratory result is validated and authorised before being sent on to the recipients. The positive results have their final authorisation by a doctor. This is enshrined in microbiology practice in the UK. The reason is because every report we issue must be seen in the clinical context. From a urine perspective, we should not simply report the presence of bacteria in the urine but seek to remind the reader of what this might mean in the clinical context. A large number of urine samples come from our older population, the same group who are being admitted with bacteraemia and which is what alerted the health board to the issue and prompted the current strategy.
When authorising the positive results, particularly in the older group, we remind our readers that asymptomatic bacteruria is common in this group and does not represent infection. This is an example of the rules above in action. Antibiotics always do harm: they always kill bacteria, primarily in the gut and lead to selection of antibiotic resistant bacteria. The positive stance we are taking (rule 2) is to nudge our readers to think about avoiding antibiotics if there are no symptoms and signs of infection. Use excess antibiotics and the bacteria in the gut and bladder will become increasingly resistant, making true infection increasingly difficult to treat. Public Health England publish a Quick Guide to managing urinary tract infection (UTI) in the community, which outlines the sort of things we are emphasising on our reports.
So what has happened locally as a result?
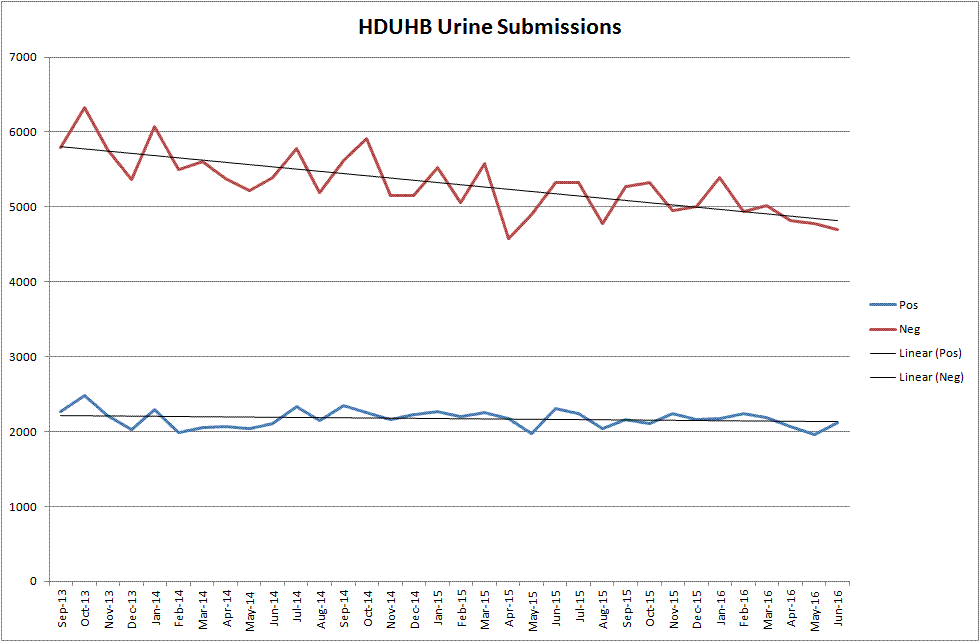
From September 2014, when we started to make increasing comments on urine reports, we have seen a fall in the number of urine samples submitted to our three laboratories. In the figure, you will see that the number of samples per month has fallen by about 1,000.
What we have found exciting about this change is that the number of positive urine samples has remained unchanged. It is the negative urines that have reduced. I believe this signals that our efforts are bearing fruit over time. Our clinical colleagues are thinking more about when is the appropriate time to submit urine samples. They are continuing to send in those that prove positive, so we do not appear to be missing the significant findings but there is a quality improvement in sampling occurring.
From a complexity standpoint, we are amplifying the positive and dampening the negative. In the next article, I will seek to show you what effect we are having on the quality of the clinical information being received on the request forms.
Leave a Reply